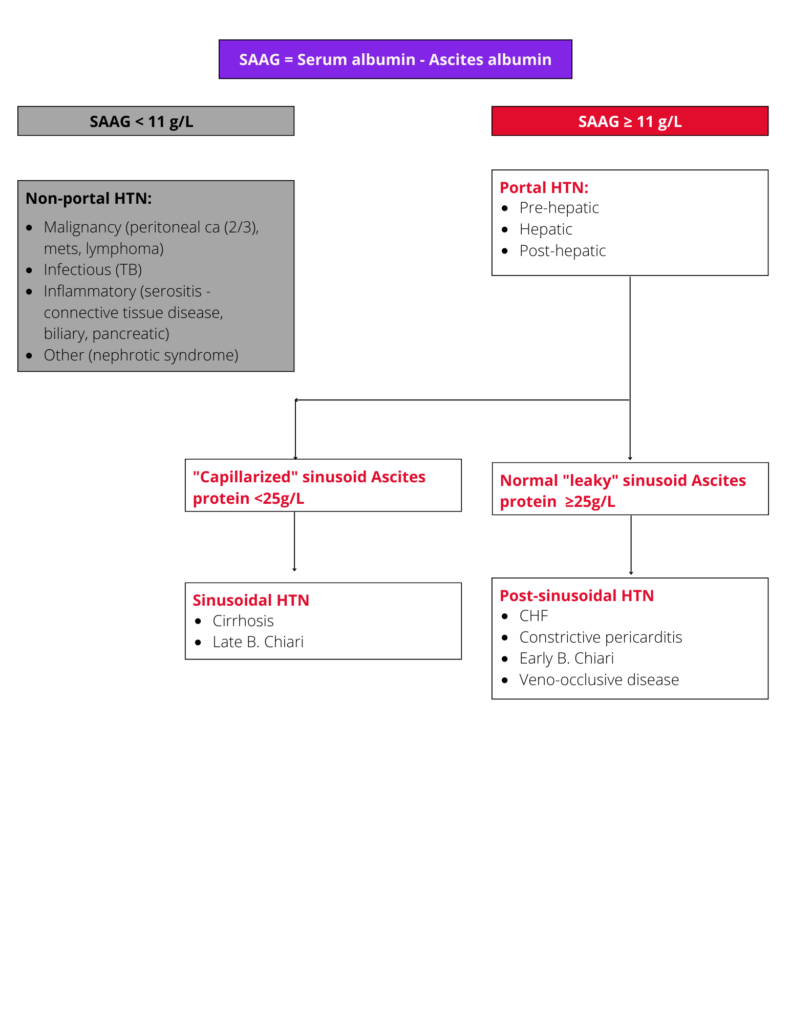
Top tips:
- Perform a diagnostic paracentesis in:
- Any patient with symptoms or signs of infection, renal dysfunction or encephalopathy.
- All patients at presentation to ER, even if asymptomatic.
- The mainstay of therapy for ascites are sodium restriction and diuretics. spironolactone and furosemide are often given in combination in a ratio of 50 mg (spironolactone) to 20 mg (furosemide). In cases of mild ascites, spironolactone monotherapy may be enough.
- Large volume paracentesis (≥ 5 L drained) is required for tense or refractory ascites. Give IV albumin (100 cc of 25% albumin (25 grams) for every 3 L ascites removed). With renal insufficiency or hypotension, be more cautious with the amount of fluid that is drained off.
- Patients with ascites may be candidates for a Transjugular intrahepatic portosystemic shunt (TIPS) or for liver transplantation.
- Non-selective beta blockers (NSBB’s) and other blood pressure lowering medications may need to be adjusted in patients with ascites
Navigation
Order panels for Ascites & Paracentesis:
For adults with cirrhosis admitted with Ascites.
Ascites Hepatic Hydrothorax, Edema in Cirrhosis Order Panel
For adult inpatient with cirrhosis requiring paracentesis.
Inpatient Cirrhosis Paracentesis Order Panel
General Cirrhosis Admission and Discharge Order Sets
*Add specific panels to general admission orders as appropriate*
For adults with cirrhosis requiring hospital admission
Cirrhosis Adult Admission Orders
For adults with cirrhosis requiring hospital discharge
Cirrhosis Adult Discharge Orders



Thank you to Dr. Tandon, Michelle Carbonneau, and Dr. Abraldes for your efforts creating the content on this page. Check out the bottom of the page for short videos from Dr. Abraldes!
A ratio of 50-100mg Spironolactone to 20-40mg Furosemide often works to balance the electrolytes, but must be individualized.
The ratio of diuretics can be adjusted to control hyperkalemia (i.e., if hyperkalemia is present, reduce Spironolactone).
If the electrolytes and creatinine are ok, doses can be increased in increments of 50mg Spironolactone to 20mg Furosemide.
For example, starting doses of Spironolactone 50mg and Furosemide 20mg can go to 100mg and 40mg respectively after 4-7 days.
#1: Dietary non-compliance - Spot urine Na/K ratio is >1 OR the 24-hour urine Na excretion is >78 mEq/day in a patient on diuretics who is not losing weight This means the patient is sensitive to diuretics but not adherent to sodium restriction.
#2: Diuretic resistance - Spot urine Na/K ratio is ≤1 OR 24-hour urinary Na excretion is <78 mEq per day in a patient on maximally tolerated diuretics who is not losing weight. This means the patient is resistant to diuretics
Introducing Dr. Abraldes, Dr. Tandon and Michelle Carbonneau
Video Links:
See relevant videos:
Video on the ultrasound based diagnosis and drainage of ascites
References:
This section was adapted from content using the following evidence based resources in combination with expert consensus. The presented information is not intended to replace the independent medical or professional judgment of physicians or other health care providers in the context of individual clinical circumstances to determine a patient’s care.
Authors: Dr. Marilyn Zeman, Dr. Guadalupe Garcia-Tsao, Dr. Vijey Selvarajah, Dr. Brian Buchanan, Dr. Puneeta Tandon
References:
- EASL Clinical Practice Guidelines for the management of patients with decompensated cirrhosis. J Hepatol 2018 Aug;69(2):406-460 PMID 29653741
- Diagnosis, Evaluation, and Management of Ascites, Spontaneous Bacterial Peritonitis and Hepatorenal Syndrome: 2021 Practice Guidance by the American Association for the Study of Liver Diseases. Hepatology (Baltimore, Md.), 74(2), 1014–1048. https://doi.org/10.1002/hep.31884 PMID 33942342
- Advancing Liver Therapeutic Approaches (ALTA) Consortium (2022). North American Practice-Based Recommendations for Transjugular Intrahepatic Portosystemic Shunts in Portal Hypertension. Clinical gastroenterology and hepatology : the official clinical practice journal of the American Gastroenterological Association, 20(8), 1636–1662.e36. https://doi.org/10.1016/j.cgh.2021.07.018 PMID 34274511
Last updated November 24, 2022